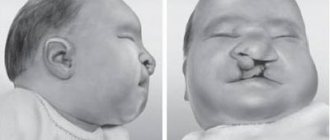
Hypocalcemia is low levels of calcium in the blood.
The medical norm is 2.2-2.5 mol/liter; when the readings are less than 1.87, this indicates the presence of a disease and requires immediate consultation with a specialist and specific treatment. The disease can be acute or chronic and develop in people of all ages, including children.
Manifestations include paresthesia, tetany, and also, in severe conditions, epileptic seizures, encephalopathy, and heart failure. Diagnosis is based on determining plasma calcium levels. Treatment of hypocalcemia includes calcium supplementation, sometimes in combination with vitamin D.
Causes of hypercalcemia
Hypercalcemia almost always indicates some disease or pathological process. However, sometimes it develops due to physiological reasons (in newborns on the 4th day of life, in adults after eating). The pathological causes of this condition are as follows:
- Hyperparathyroidism.
This is an endocrine disease characterized by hypersecretion of parathyroid hormone (PTH). It is the most common cause of hypercalcemia. Hyperparathyroidism is caused by adenoma, hyperplasia of the parathyroid glands, and renal failure. Sometimes hyperparathyroidism occurs as part of autoimmune polylinglandular syndrome or multiple endocrine neoplasia. - Oncological diseases.
Recognized as the second most common cause of this electrolyte disorder. In cancer, it occurs through two mechanisms. The first is bone destruction by metastases or primary focus (leukemia, lymphoma, myeloma). The second mechanism is the synthesis of PTH-like peptide by cancer cells (lung, breast, bladder cancer). - Granulomatous processes.
Chronic diseases characterized by the formation of cellular granulomas in tissues (primarily in the lungs) can also cause hypercalcemia. These include tuberculosis, sarcoidosis, histoplasmosis. Mononuclear phagocytes that are part of granulomas, due to the expression of 1-alpha hydroxylase, are able to convert vitamin D into the active form (calcitrirol, 1,25OH-D3), which enhances the absorption of calcium ions by the small intestine. - Prolonged immobilization.
As a result of prolonged inactivity, osteoclasts (cells that destroy bone tissue by dissolving mineral compounds) are activated. This leads to the release of calcium ions from the bones. This phenomenon occurs during forced immobilization after injuries, being in conditions of weightlessness (during space flights). - Taking medications.
This primarily applies to vitamin D and calcium supplements. Other medications (thiazide diuretics, theophylline, lithium) can also cause calcium imbalance by increasing osteodestruction or reabsorption processes in the tubules of the nephrons of the kidneys. - Other endocrine disorders.
In addition to the pathology of the parathyroid glands, other endocrine diseases are sometimes the cause of hypercalcemia. For example, an excess of thyroid hormones in hyperthyroidism increases the destruction of bone tissue. With adrenal insufficiency, the inhibitory effect of glucocorticoids on calcium metabolism is reduced.
Lack of calcium in the body symptoms in women
The body of the fair half of humanity is protected by nature from the loss of calcium with the help of estrogens. They help preserve it in bones and enamel, so hormonal changes directly affect the development of deficiency.
During pregnancy, a woman has to consume calcium not only for the needs of her own body, but also to supply the baby for normal growth and development. Moreover, nature is quite cunning - if the nutrient is not enough, then it will use all its strength to preserve the fetus, actively taking reserves of the substance from the bones and teeth. This is why expectant mothers’ teeth quickly decay during pregnancy.
The signs of hypocalcemia in women are practically no different from those in men. The only difference is the change in the flow of menstruation. The phenomena of PMS intensify - increased pain during menstruation, cycle disruption (if women have not had any problems before).
Fact: not only calcium supplements, but also the introduction of magnesium and vitamin B6 supplements into the diet will help ease the course of PMS (premenstrual syndrome). These supplements will greatly reduce the dose of non-steroidal drugs.
Pathogenesis
An increase in calcium content in the blood changes the membrane potential of cells, which leads to inhibition of neuromuscular conduction in skeletal muscles, myocardium, and the gastrointestinal tract. The pathogenesis of neuropsychiatric symptoms is not completely clear. The role of slowing down the conduction of nerve impulses is assumed. Calcification of blood vessels, internal organs, dystrophy, and tissue shrinkage develops.
Due to hypercalciuria (increased filtration of calcium in the nephron tubules), the risk of nephrolithiasis increases. Calcium inhibits adenylate cyclase, which suppresses the renal effect of antidiuretic hormone. Also, due to the high extracellular concentration of this cation, the secretion of hydrochloric acid by the lining cells of the stomach increases, which leads to the development of peptic ulcers.
Consequences of hypocalcemia
Calcium deficiency in the body leads to growth retardation, rickets in children, scoliosis, allergies, bone curvature, blood clotting disorders, the formation of kidney stones, and capillary fragility.
People suffering from chronic calcium deficiency have difficulty withstanding physical and mental stress and are susceptible to infections; their teeth decay, their gums bleed, and convulsions occur.
The most severe diseases caused by calcium deficiency are osteoporosis and osteomalacia, characterized by softening of the bones.
A lack of calcium can cause multiple sclerosis. If the required amount of calcium does not enter the human body before the age of 15, this leads to weakening of the nervous tissue and an increased risk of developing multiple sclerosis.
Thus, hypocalcemia is a pathological condition of the body, which, in the absence of appropriate treatment (use of calcium supplements, vitamin D) can lead to serious illnesses and a reduction in life expectancy. Therefore, it is so important to eat rationally and promptly treat diseases that can lead to the development of hypocalcemia.
Classification
According to the current, chronic and acute hypercalcemia (hypercalcemic crisis) are distinguished. Based on the level of cation (in mmol/l), the following degrees of severity of hypercalcemia are distinguished:
- Easy.
The content of total Ca is less than 3, ionized Ca is less than 1.5. - Moderate.
The level of total Ca is up to 3.5, ionized - up to 1.8. - Heavy.
Total Ca is above 3.5, ionized Ca is more than 1.8.
Pseudohypercalcemia is considered separately. Part of the calcium binds to plasma proteins, therefore diseases such as paraproteinemic hemoblastoses (multiple myeloma), characterized by a high protein content in the blood, are accompanied by an increase in the level of total calcium. Determination of ionized calcium helps to exclude false hypercalcemia.
Children drink milk
This phrase from the song of the Soviet cartoon is known even to those who have never seen it. Cow's milk does have a high calcium content, but its role is significantly overrated. After all, in order to cover the body’s expenditure on the mineral, it is necessary to consume at least 1 liter every day, and to obtain the necessary calcium for pregnant women, even more – about 2 liters.
But that's not the problem with whole milk. Pediatricians do not recommend giving it to children under one year of age due to the high likelihood of developing allergies and the high concentration of phosphorus, which the child’s body has difficulty removing, wasting calcium reserves on its utilization. As a result, the problem turns into a vicious circle.
By the way, the famous pediatrician Dr. Komarovsky, in his recommendations, suggests giving up whole milk altogether for children under 3 years of age. In order not to provoke increased leaching of the element. At an older age, the enzymatic and digestive systems are fully formed, so this product no longer carries such a high risk of calcium loss.
Recent US studies have found an increased likelihood of developing the risk of prostate and ovarian tumors. More than 10 thousand people participated in the data collection; according to statistics, the incidence of ovarian cancer in women increased by 2 times with regular consumption of at least 4 servings of whole milk. For men, the numbers are slightly lower - the number of pathologies increased by an average of 30%.
The main role in provoking tumor diseases is played by insulin-like growth factor and estrogens, which are contained in milk. At the same time, cheese and fermented milk products do not cause such changes, since the enzymatic processing of these substances is largely destroyed.
Of course, you shouldn't completely exclude milk from your diet. It is enough to combine it with other sources of calcium. Also, you should not get carried away with low-fat foods, as this will deprive yourself of important fat-soluble vitamins - A, E and D, which also have high antioxidant activity.
Symptoms of hypercalcemia
With a mild degree of pathology, there may be no symptoms at all. In moderate to severe cases, muscle weakness appears, sometimes reaching such severity that it is difficult for the patient to get out of bed. Symptoms from the gastrointestinal tract are typical - nausea, vomiting and abdominal pain. Appetite decreases significantly and constipation occurs. Cardiac symptoms (increased blood pressure, tachycardia) are often observed.
Even with hypercalcemia of non-oncological origin due to anorexia and muscular dystrophy, the patient loses a lot of weight, acquires a cachectic appearance, which may give a false impression that he has a malignant neoplasm. The weakening of the effect of antidiuretic hormone on the kidneys causes the appearance of symptoms such as severe thirst, an increase in urine output to 5-6 liters per day.
Neuropsychological symptoms are especially clearly presented. First, emotional instability, impaired concentration, and slight drowsiness occur. In severe cases of pathology, confusion, delirium, and psychosis develop. Hallucinations are possible. With long-term high levels of calcium, it begins to be deposited in the tissues of the joints (chondrocalcinosis), which causes arthralgia.
Complications
Hypercalcemia has a wide range of adverse effects. The most common complications are osteoporosis (due to increased release of calcium ions from bones), pathological fractures, and urolithiasis. Acute pancreatitis and intestinal obstruction occur less frequently. The most life-threatening condition is considered to be hypercalcemic crisis, in which mortality reaches 60%. The cause of death is heart or kidney failure.
Another severe but rare complication is calciphylaxis (calcifying uremic arteriolopathy), characterized by ischemic necrosis of the skin and subcutaneous fat. It develops in patients with end-stage renal failure. A prolonged increase in calcium in the blood can also lead to band keratopathy, calcification of the aorta and heart valves with the formation of heart defects.
Diagnostics
The profile of a medical specialist supervising a patient with this pathology is determined by the cause that caused this condition. Most often, such patients are seen by endocrinologists, nephrologists, and oncologists. When interviewing the patient, it is necessary to clarify what medications he is taking. During the examination, the doctor pays attention to symptoms such as decreased muscle tone and suppressed tendon reflexes. An additional examination is prescribed, including:
- Laboratory research.
A biochemical blood test measures the level of albumin, urea, and creatinine. Of the electrolytes, in addition to total and ionized Ca, the concentration of phosphorus and chlorides is determined. The content of vitamin D (25OH-D) is studied. PTH, PTH-like peptides. Daily urinary Ca excretion is checked. If thyrotoxicosis or hypocortisolism is suspected, a blood test for hormones (TSH, free T4, cortisol) is performed. - Functional tests.
Special provoking tests provide invaluable assistance for differential diagnosis of the causes of this disorder. These include tests with native vitamin D, thiazide diuretics, and calcitonin. A steroid suppression test with prednisolone can be used to exclude a process not associated with increased PTH secretion. - Instrumental research.
To search for adenoma or hyperplasia of the parathyroid glands, ultrasound, computed tomography, and scintigraphy are performed. Densitometry is performed to determine bone mineral density, and renal ultrasound is performed to diagnose nephrolithiasis. If there are symptoms that raise suspicion of an inflammatory process in the lungs or a malignant neoplasm, radiography, CT scan of the lungs, abdominal organs, and mammography should be prescribed to identify them.
Differential diagnosis must be made based on the predominant symptoms. Insipidal syndrome must be differentiated from diabetes mellitus and diabetes insipidus. Muscle weakness and hypotension should be distinguished from that with muscular dystrophies, myasthenia gravis, and polymyositis. Neuropsychiatric symptoms require the exclusion of psychiatric diseases.
Scintigraphy. Parathyroid adenoma
Treatment of hypercalcemia
Conservative therapy
Patients with any degree of severity should be hospitalized in a hospital (endocrinology, nephrology department) for treatment. Patients with severe neurological symptoms and hypercalcemic crisis should be transferred to the intensive care unit. It is necessary to discontinue all medications that can cause an increase in calcium levels. Treatment of hypercalcemia has the following directions:
- Increased excretion of calcium in urine.
First, it is necessary to ensure adequate rehydration with physiological NaCl solution (0.9%). This will improve renal perfusion and increase the filtration of calcium ions by the renal glomeruli. Additionally, forced diuresis is performed using loop diuretics (furosemide). It is necessary to constantly monitor blood electrolyte levels. - Decreased absorption of Ca in the intestine.
Sodium or potassium phosphate salts are well suited for this purpose. Phosphates are strictly contraindicated for the treatment of secondary hyperparathyroidism caused by renal failure. Also, glucocorticosteroids (prednisolone, hydrocortisone) and synthetic antimalarial drugs (hydroxychloroquine, chloroquine) are used to suppress Ca absorption in the gastrointestinal tract. - Suppression of bone resorption.
An important stage in the treatment of hypercalcemia caused by hyperparathyroidism or cancer. The most effective drugs for preventing the progression of osteoporosis are bisphosphonates (pamidronic acid, zoledronic acid), which inhibit the activity of osteoclasts. The peptide hormone calcitonin and the cytotoxic antibiotic mithramycin have a similar mechanism of action, but a faster effect. - Suppression of the production of PTH and PTH-like protein.
For the pathogenetic treatment of primary and secondary hyperparathyroidism, calcimimetics (cinacalcet) are used, which increase the sensitivity of PTG cell receptors, thereby reducing PTH production. Gallium nitrate is used to treat hypercalcemia caused by a malignant tumor, which inhibits the secretion of PTH-like protein by tumor cells. - Intensive therapy.
For the treatment of severe life-threatening conditions (hypercalcemic crisis, calciphylaxis), as well as when other conservative methods of therapy are ineffective, hemodialysis using a low-calcium dialysate solution is an emergency measure to reduce Ca in the serum.
Surgery
Surgical removal of the parathyroid glands is the main treatment for primary hyperparathyroidism. The main indication for surgical intervention is a Ca level above 2.75 mmol/l. To prevent postoperative hypocalcemia (“hungry bone syndrome”), the patient is prescribed vitamin D and calcium supplements. Malignant tumors also need to be removed. To treat oncohematological pathologies, bone marrow transplantation is performed.
Experimental treatment
New drugs are currently being developed to treat this condition. The drug osteoprotegerin, which is a cytokine from the family of tumor necrosis factors, is at the stage of clinical trials. It inhibits the differentiation of osteoclasts and stimulates their apoptosis. In in vitro experiments, the calcitriol analogue EB 1089 suppressed the expression of the PTH peptide gene.
Symptoms and signs of hypocalcemia
- Impaired wakefulness, attention and concentration
- Seizures
- Paresthesia, tetany
- Confusion, states of fear, agitation, hallucinations, depression
- Chorea syndrome and Parkinson's syndrome in chronic hypocalcemia
- AV block, circulatory arrest
Moderate hypocalcemia is usually asymptomatic, but when severe, the so-called classic tirade occurs: carpopedal spasm, stridor and convulsions. In this case, a characteristic spasm of the hand (“obstetrician’s hand”) is observed. Tingling sensations appear in the area of the hands and feet, as well as around the mouth. A tendency to cramps in the hands can be identified by artificially reducing their blood supply: to do this, apply a tonometer cuff as usual and compress the artery for 3 minutes. As a result, a characteristic spasm of the hand develops (Trousseau's symptom). Less reliably reveals a hidden tendency to convulsions. Chvostek's symptom - when you tap the area where the facial nerve exits with your finger, spasms of the facial muscles occur on the same side. According to the results of the ECG, the Q-T interval may lengthen, which predisposes to the development of ventricular arrhythmia. Long-term hypocalcemia and hyperphosphatemia (eg, hypoparathyroidism) can cause cataracts, basal ganglia calcification, and epilepsy. Hypocalcemia and hypophosphatemia associated with vitamin D deficiency in adults cause osteomalacia.
Hypocalcemia is often asymptomatic. The main clinical manifestations of hypocalcemia itself are associated with changes in the membrane potential of cells, causing neuromuscular excitability.
Neurological manifestations . Spasms of the muscles of the back and legs often occur.
Tetany is typically associated with severe hypocalcemia, but also occurs with a decrease in only the ionized fraction of Ca in the absence of obvious hypocalcemia.
Tetany can be either obvious, manifested by spontaneous symptoms, or latent, which is detected only with the help of provocative manipulations. Latent tetany usually occurs with a smaller decrease in serum Ca concentration.
Other manifestations . Chronic hypocalcemia is also characterized by other manifestations: dry and flaky skin, brittle nails and coarse hair. Sometimes candidal infections develop (especially often with idiopathic hypoparathyroidism). With prolonged hypocalcemia, cataracts are also observed, and correction of the level of Ca in the serum does not lead to its reverse development.
Prognosis and prevention
Hypercalcemia is a severe and in some cases (especially in acute cases) a life-threatening pathological condition. In hypercalcemic crisis, the mortality rate is very high (60%). The frequency of deaths in chronic cases averages 20-25%. However, the prognosis is largely determined by the cause of the increase in Ca levels.
Prevention of this pathology consists in timely diagnosis and proper treatment of the diseases against which it develops. Before starting to take vitamin D or other medications that may increase Ca levels in the blood, a blood test should be performed to assess Ca levels.
What foods contain calcium
If the symptoms of hypocalcemia are in the early stages, without progressing to serious clinical diseases, then the deficiency can be successfully eliminated by introducing a list of calcium-rich foods into the diet.
The best known sources of the mineral are dairy products. Sufficient consumption of cottage cheese and cheese allows you to fill the body’s daily needs. For example, in order for an adult to get his daily requirement, it is enough to eat 160 grams of cream cheese (this is in the complete absence of Ca in other menu products). The element obtained from milk is well absorbed by the body, and such food is an excellent source of protein.
But not only “milk” can cover the body’s needs, especially since there is a significant segment of the population with lactase deficiency (intolerance to the milk sugar lactose). Many vegetarians also avoid dairy products. In this case, cabbage, spinach, and nuts are valuable sources.
List of foods rich in calcium
| Name | Amount of calcium per serving (mg) | Serving size in grams |
| Eggs | 30 | 1 PC |
| Sardines in oil | 235 | 60 |
| Beans | 130 | 200 gr. boiled |
| Chickpeas | 98 | 200 gr. boiled |
| Parsley and dill | Approximately 200 mg | 100 |
| Sea kale | 80 | 100 |
| White cabbage, cauliflower, broccoli | 130 mg | 200 |
| Spinach | 50 | 100 |
| Garlic | 180 | 100 |
| Prunes | 145 | 120 |
| Dried apricots | 65 | 120 |
| Oranges | 60 | 150 |
| Almond | 75 | 30 |
| Ice cream (made from natural cream, not vegetable fats) | 125 | 100 |
| Cottage cheese | 140 | 200 |
| Cheese | 180 | 30 |
| Milk | 240 | 200 ml |
| Yogurt | 210 | 150 ml |
As can be seen from the table, a lot of Ca is found not only in well-known dairy products. It can easily be replenished from quite affordable ordinary greens, legumes, and canned fish. Seafood, by the way, is recommended to be consumed without fail if there is a lack of calcium, as a source of vitamin D.
Up to 50 years of age, natural food is absorbed almost completely, enriching the body with the necessary mineral, but this applies to healthy people.